Our innovation projects
North Central London Cancer Alliance is involved in a range of exciting innovation projects. Here are just some of them.
Ovarian cancer surveillance
University College London Hospitals NHS Foundation Trust (UCLH), in collaboration with the North Central London Cancer Alliance and GENinCode Plc, is the first hospital trust in the UK to provide an ovarian cancer surveillance testing service as part of its Familial Cancer Clinic. The service is for women who have a high risk of ovarian cancer due to inherited BRCA1 or BRCA2 gene alterations, who wish to defer preventative surgery. Surveillance is possible due to the Risk of Ovarian Cancer Algorithm (ROCA) Test. This is a proprietary algorithm that calculates a woman’s individual risk based on several factors, including a four-monthly blood test.

COMPASS

The COMPASS (Community Pharmacy Assessment for Barrett’s Oesophagus and Reflux Symptoms) project aims to use capsule sponge tests to identify undiagnosed patients with Barrett’s oesophagus and early-stage oesophageal adenocarcinoma.
A key part of the project is to identify patients in community pharmacy settings and establish referral routes into community-based clinics for testing.
MENO.pause app
The Alliance part-funded the development of MENO.pause, a digital decision-making aid to help clinicians manage menopause symptoms. It is supported by patient groups and menopause organisations.
Doctors at UCLH and University College London (UCL) developed MENO.pause for use in primary care and hospital settings, promoting improved local access to high quality menopause advice, reducing the need for unnecessary tests or hospital visits.
The app also supports women with complex health conditions, providing options for those receiving cancer treatment, which may cause early menopause, and those with genetic variations which put them at higher risk of cancer.

Radiotherapy organ contouring
UCLH radiotherapy, supported by the North Central London Cancer Alliance, adopted Limbus-AI, a neural network-based auto-contouring software, that aids oncologists in planning radiotherapy for their patients.
During radiotherapy planning the oncologists must identify organs at risk to protect from radiotherapy. This is done by using a CT scan and was previously a lengthy process, but Limbus-AI saves clinicians over 30 minutes for every case.
It has also improved workflow efficiency. Since its implementation, the days taken to plan have significantly decreased. By automating a previously repetitive, manual process, clinicians now have more time to focus on planning radiotherapy towards the cancer and other clinical work.
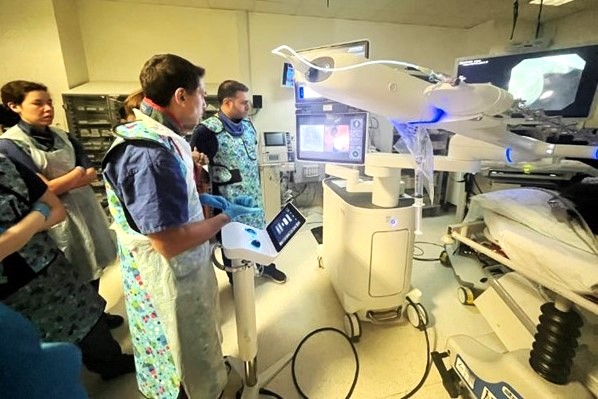
Navigational robotic bronchoscopy
As part of the North Central London Cancer Alliance Innovation Fund 2023-24, UCLH piloted a programme of robotic bronchoscopies to improve early diagnosis rates in lung cancer, especially in those unsuitable for a traditional CT scan.
Robotic bronchoscopy detects early lung cancer with high precision and has demonstrated practical benefits in streamlining the diagnostic pathway and detecting more lung cancers earlier. In 140 procedures over nine months, the successful diagnosis rate was 80%.
The service was further awarded an National Institute for Health and Care Research (NIHR) grant of nearly £800,000. The Alliance is also continuing to fund the expansion of navigational bronchoscopy.
Virtual reality training for cancer care professionals
The Alliance has awarded funding to teams at UCLH to reshape how cancer care professionals are trained in essential clinical communication skills with patients.
Using immersive virtual reality technology, staff will be able to practise sensitive conversations – like breaking bad news or supporting distressed patients – in a realistic, low-pressure environment.
Recruitment of participants for this two-year project began in November 2025.
WID-easy
Endometrial cancer is the fourth most common cancer in UK women and is rising due to increasing obesity levels and longer life expectancy.
We supported a successful grant application to the NIHR i4i Product Development Award to fund the EASY-CARE study. This study will trial an innovative swab test for womb cancer in four North Central London hospitals.
Benefits of the test include a better patient experience, by reducing the number of women requiring hysteroscopy, with the potential for self-testing in future, and reduction in health inequalities, with ultrasounds having significantly lower sensitivity for Black populations than the WID-easy test.
