Lung Cancer Screening
Frequently Asked Questions

These FAQs provide information for healthcare professionals about Lung Cancer Screening and help with answering patients' questions.
There are often no signs or symptoms of lung cancer at an early stage. As a result, sadly 7 out of 10 cancer patients are diagnosed too late to be cured. Lung Cancer Screening can help diagnose lung cancer early, at a stage where treatment can be simpler and more successful.
Lung Cancer Screening is a two stage process to help assess the health of a patient’s lungs. It begins with a telephone call or meeting where a member of the screening team will ask a series of questions to evaluate the patient’s chances of developing lung cancer. If they are identified as someone who is at an increased risk of developing lung cancer they will be invited for a quick scan to produce a detailed image of the lungs.

Data from the screening programme so far shows that with these potentially life-saving checks, lung cancer early diagnosis rates can be as high as 80% – compared to less than 30% without this type of intervention – enabling doctors to treat cases sooner, when curative treatment is more possible, saving more lives.
Patients aged 55 to 74 who have ever smoked will be invited for Lung Cancer Screening, providing their smoking status is correctly recorded in their GP record.
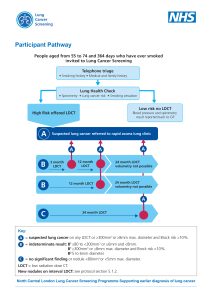
The lung health check comprises of two stages: First a telephone call with a member of the Lung Cancer Screening team who will carry out a brief assessment of the patient’s risk of lung cancer. Secondly, if deemed to be high risk the patient will be invited for an appointment at University College Hospital, Finchley Memorial Hospital or the Community Diagnostic Centre in The Mall Wood Green.
At the Lung Cancer Screening appointment, a health care professional will ask the patient a series of questions about their smoking history, lifestyle and current health and wellbeing and complete a risk assessment based on the answers given by the participant. If the patient meets a certain risk threshold on the risk assessment, they will be offered a low dose CT scan.
Information for those eligible for screening is available on a dedicated website – lungchecklondon.org. If patients have questions about having Lung Cancer Screening and cannot find the answer on the website or in their invitation letter, they can email: uclh.ncllunghealthcheck@nhs.net or call 0800 652 9589.
The possible outcomes of a CT scan are covered on page 6 of the Patient Information Booklet.
GPs will be informed by letter about clinically actionable findings to be followed up in either primary or secondary care.
Download NCL Clinically actionable findings
There are a number of reasons why a patient might not be offered a
low dose CT scan and these include:
• They’re unable to lie flat
• They’re unable to transfer onto the CT scanning bed without
support, or with the support of somebody who attends the scan
with them
• They weigh more than 200kg/31.5 stones
• They are not physically fit
• They do not have capacity to consent to the CT scan and it is not
in their best interests to have one
CT scans for Lung Cancer Screening take place at University College Hospital, Finchley Memorial Hospital and the Community Diagnostic Centre in The Mall Wood Green.
Across England up to 1.5m people will be invited for Lung Cancer Screening.
Lung Cancer Screening is being rolled out as a national programme from April 2025 onwards. This follows the recommendation made by the UK National Screening Committee in 2022.
The CT scan appointment
Yes, this may be possible. Patients should ask the Lung Cancer Screening team for further information. Contact details will be in their invitation letter.
Patients will need to remove clothes on their top half for the CT scan. They will be given a hospital gown.
The CT scan appointment is explained in the Patient Information Booklet and on the website www.lungchecklondon.org
Yes, support is available for people with additional needs. The Lung Cancer Screening team will be able to provide further information on the support available.
Invitation letters will be sent to the patient’s registered address that is held by their GP practice.